Hip Bursitis or Gluteal Tendinopathy?
Understanding Greater Trochanteric Pain Syndrome (GTPS) and Lateral Hip Pain
Pain on the outside of your hip is often labelled “hip bursitis.” However, research now shows that while the bursa can be involved in some cases, the source of symptoms is usually related to the gluteal tendons.
So what’s really going on?
What is Bursitis?
Bursae are small, fluid-filled sacs that cushion and lubricate the space between tendons and bones. They produce synovial fluid — a nourishing lubricant that helps joints move smoothly.
Bursitis (like tonsillitis or arthritis) refers to inflammation of a bursa. It can be caused by:
-
Sudden trauma
-
Sustained compression
-
Repetitive or cumulative overload
Hip Bursitis vs Greater Trochanteric Pain Syndrome (GTPS)
Pain on the outside of the hip is commonly diagnosed as bursitis based on ultrasound reports or GP referrals. However, we know when imaging is undertaken structural changes to bursa are common even in people without hip pain.
Given multiple structures can cause pain in this area, the condition has been re-categorised as:
Greater Trochanteric Pain Syndrome (GTPS)
The greater trochanter is the large bony prominence on the outside of your hip where the lateral gluteal muscles attach.
Research shows the gluteus medius and gluteus minimus tendons are the predominant culprits— not the bursa.
This is why you may also hear the term:
Gluteal tendinopathy
(Confusing, I know!)
Greater Trochanteric Pain Syndrome (GTPS) FAQs
What are the common symptoms of GTPS?
-
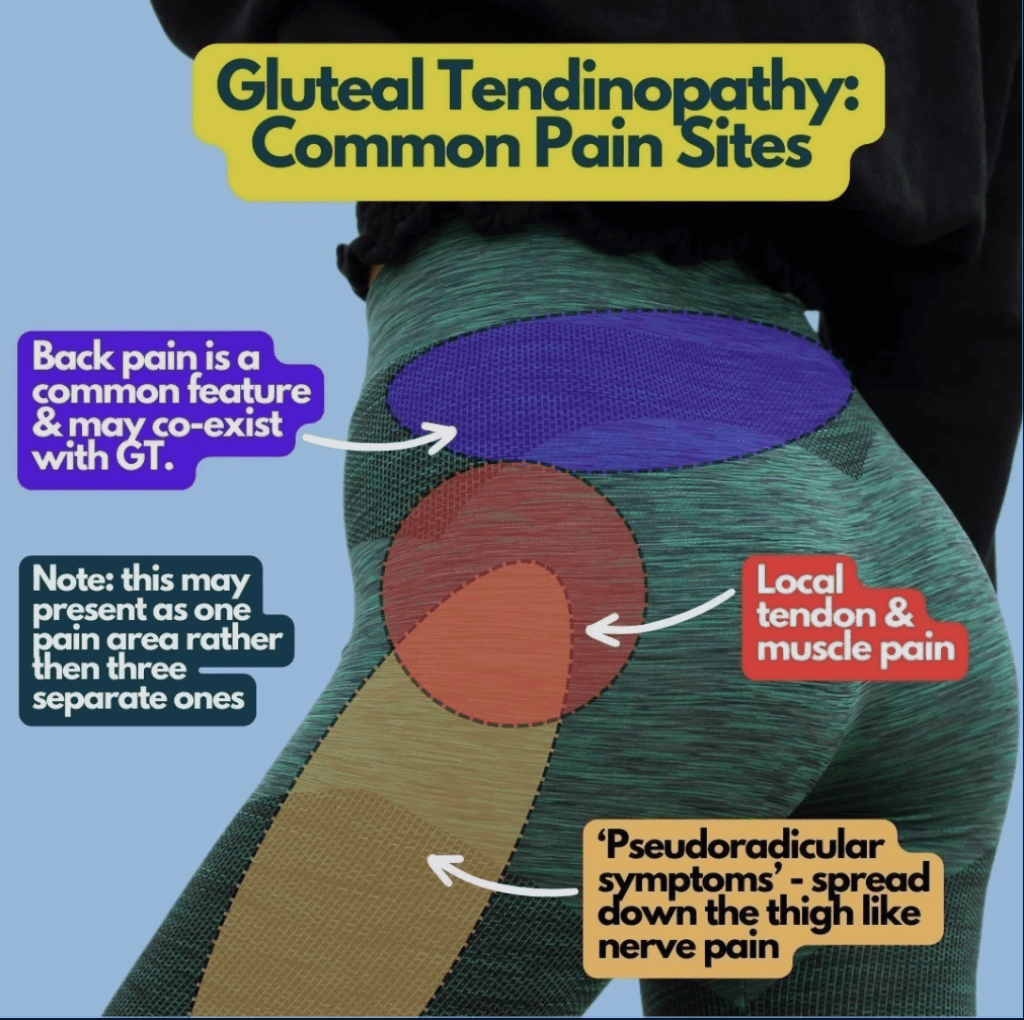
Pain on the outside (lateral) hip that can refer into the lateral thigh or even leg. These symptoms are commonly aggravated by different types of forces, and include:
Compressive load
-
Lying on the affected side
-
Sitting with legs crossed
- Sitting long periods
Contractile load
-
Running
-
Climbing stairs
-
Sudden increases in activity
When the total load exceeds the tendon’s capacity, it can trigger a ‘failed healing response’ (Tendinopathy or tendinopathy on scans) leading to pain, weakness, and further impairment.
How is GTPS diagnosed?
A thorough clinical examination is sufficient to diagnose GTPS. Imaging is not routinely required; however, many people will still prefer to obtain a scan.
If necessary:
-
Ultrasound can visualise tendon changes
-
Further investigations may be requested if your therapist or GP suspects red flags are present (this is important!)
Red flags may include:
-
Trauma or fracture
-
Inflammatory conditions
-
Avascular necrosis (associated with prolonged corticosteroid use or excessive alcohol intake)
Who is at risk of lateral hip pain / GTPS?
-
Menopausal women
-
Athletes with sudden spikes in training load
-
Sedentary workers sitting for prolonged periods
What treatment works for hip bursitis or gluteal tendinopathy?
Education
Understanding load management and positions to avoid is essential.
Activity modification
Not complete rest — but strategic de-loading.
This may include:
-
Reducing running volume
-
Avoiding lying on the painful side
-
Breaking up prolonged sitting
-
Using a standing desk
Progressive strengthening
Restoring tendon load capacity is critical with any tendon rehab (there is no short-cuts!).
Rehabilitation typically progresses from:
-
Isometric exercises (static contractions)
-
Heavy slow strengthening
-
Functional or plyometric exercises (depending on goals)
Do I need a cortisone injection for hip bursitis?
Initially, no.
Research into injection therapy remains inconclusive and is not initially recommended. Suitability should be discussed with your GP or Sports Physician.
I have a tendon tear — is it safe to exercise?
Yes.
Tendinopathies progress through stages, and degenerative tendons can show permanent structural changes such as small tears.Graduated, structured loading is not only safe — it is essential to restore tendon capacity.
Exercise aggravates my hip pain. Where do I start?
This varies between individuals, which is why consulting a Physiotherapist to determine your starting point is important.
Isometric exercises (static contractions) in a neutral hip position are often a good entry point for many people and can be progressed as your symptoms reduce and strength improves.
Mild pain up to 3/10 that settles quickly and does not worsen over 24 hours is generally acceptable for tendon pain.
Does stretching help lateral hip pain?
No.
Although stretching feels logical for a tight, painful area, it adds compressive load to the tendon and can aggravate symptoms.
When should I get a scan for hip pain?
Scans should be reserved for:
-
Suspicious red flags (e.g. fracture)
-
Lack of improvement with conservative treatment
Ultrasound is generally a first stating point to visualise the gluteal tendons while x-ray can assess the hip joint or lumbar spine which can both refer pain to the lateral hip.
How long does GTPS take to recover?
Recovery time varies; however, research shows that 12+ weeks is common.
Clinically, many patients experience significant symptom improvement once they understand load management and begin structured rehabilitation.
Outside Hip Pain? Book a Physiotherapy Assessment
If you have pain on the outside of your hip — whether diagnosed as hip bursitis, GTPS, or gluteal tendinopathy — a thorough clinical assessment is essential.
The solution is not rest.
It is modifying your activities in the short term and undertaking structured, progressive loading
Book an appointment to commence a safe, individualised rehabilitation plan.
References
Pumarejo Gomez L, Li D, Childress JM. Greater Trochanteric Pain Syndrome (Greater Trochanteric Bursitis) [Updated 2024 Feb 25].
McMillan (2018). Greater Trochanteric Pain Syndrome (GTPS): Assessment & Management. https://semrc.blogs.latrobe.edu.au/wp-content/uploads/2018/05/RMcMillan_GTPS.pdf